Abstract
Introduction
Treatment of posterior pelvic ring injuries is frequently associated with pain or/and high mortality rates. Percutaneous sacro-iliac (SI) screw fixation has proved to be one of the methods of choice, providing minimal operative time, blood loss and wound-related morbidity. However, fixation failures due to secondary fracture dislocation or screw backing out have been reported. There is a little knowledge regarding the impact of varying screw orientation and quality of reduction on the fixation strength.
Purpose
The purpose of the present study was biomechanical investigation of joint stability after SI screw fixation and its dependence on quality of reduction and screw orientation.
Methods
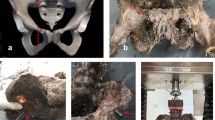
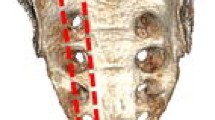
Thirty-two artificial hemi-pelvices were assigned to four study groups and simulated SI dislocations were fixed with two SI screws in oblique or transverse screw orientation and anatomical or non-anatomical reduction in group A (oblique/anatomical), B (transverse/anatomical), C (oblique/non-anatomical) and D (transverse/non-anatomical). Mechanical testing was performed under progressively increasing cyclic axial loading until fixation failure. SI joint movements were captured via optical motion tracking. Fixation performance was statistically evaluated at a level of significance p = 0.05.
Results
The highest cycles to failure were observed in group A (14038 ± 1057), followed by B (13909 ± 1217), D (6936 ± 1654) and C (6706 ± 1295). Groups A and B revealed significantly longer endurance than C and D (p ≤ 0.01).
Conclusions
Different screw orientations in the presented model do not influence substantially SI joint stability. However, anatomical reduction is not only mandatory to restore a malalignment, but also to increase the SI screw fixation strength and prevent fixation failures.





Similar content being viewed by others
References
Poenaru DV, Popescu M, Anglitoiu B, Popa I, Andrei D, Birsasteanu F (2015) Emergency pelvic stabilization in patients with pelvic posttraumatic instability. Int Orthop 39(5):961–965. doi:10.1007/s00264-015-2727-5
Tile M (1988) Pelvic ring fractures: should they be fixed? J Bone Joint Surg Br 70(1):1–12
Berber O, Amis AA, Day AC (2011) Biomechanical testing of a concept of posterior pelvic reconstruction in rotationally and vertically unstable fractures. J Bone Joint Surg Br 93(2):237–244. doi:10.1302/0301-620X.93B2.24567
Leighton RK, Waddell JP, Bray TJ, Hapman MW, Simpson L, Martin RB, Sharkey NA (1991) Biomechanical testing of new and old fixation devices for vertical shear fractures of the pelvis. J Orthop Trauma 5(3):313–317
Shuler TE, Boone DC, Gruen GS, Peitzman AB (1995) Percutaneous iliosacral screw fixation: early treatment for unstable posterior pelvic ring disruptions. J Trauma 38(3):453–458
Keating JF, Werier J, Blachut P, Broekhuyse H, Meek RN, O’Brien PJ (1999) Early fixation of the vertically unstable pelvis: the role of iliosacral screw fixation of the posterior lesion. J Orthop Trauma 13(2):107–113
van Zwienen CM, van den Bosch EW, Hoek van Dijke GA, Snijders CJ, van Vugt AB (2005) Cyclic loading of sacroiliac screws in Tile C pelvic fractures. J Trauma 58(5):1029–1034
Routt C Jr, Meier MC, Kregor PJ, Mayo KA (1993) Percutaneous iliosacral screws with the patient supine technique. Oper Tech Orthop 3(1):35–45
Sagi HC, Ordway NR, DiPasquale T (2004) Biomechanical analysis of fixation for vertically unstable sacroiliac dislocations with iliosacral screws and symphyseal plating. J Orthop Trauma 18(3):138–143
Carlson DA, Scheid DK, Maar DC, Baele JR, Kaehr DM (2000) Safe placement of S1 and S2 iliosacral screws: the “vestibule” concept. J Orthop Trauma 14(4):264–269
Citak M, Hufner T, Geerling J, Kfuri M Jr, Gansslen A, Look V, Kendoff D, Krettek C (2006) Navigated percutaneous pelvic sacroiliac screw fixation: experimental comparison of accuracy between fluoroscopy and Iso-C3D navigation. Comput Aided Surg: Off J Int Soc Comput Aided Surg 11(4):209–213. doi:10.3109/10929080600890015
Bergmann G, Deuretzbacher G, Heller M, Graichen F, Rohlmann A, Strauss J, Duda GN (2001) Hip contact forces and gait patterns from routine activities. J Biomech 34(7):859–871
Gueorguiev B, Ockert B, Schwieger K, Wahnert D, Lawson-Smith M, Windolf M, Stoffel K (2011) Angular stability potentially permits fewer locking screws compared with conventional locking in intramedullary nailed distal tibia fractures: a biomechanical study. J Orthop Trauma 25(6):340–346. doi:10.1097/BOT.0b013e3182163345
Windolf M, Muths R, Braunstein V, Gueorguiev B, Hanni M, Schwieger K (2009) Quantification of cancellous bone-compaction due to DHS Blade insertion and influence upon cut-out resistance. Clin Biomech (Bristol, Avon) 24(1):53–58. doi:10.1016/j.clinbiomech.2008.09.005
Gardner MJ, Morshed S, Nork SE, Ricci WM, Chip Routt ML Jr (2010) Quantification of the upper and second sacral segment safe zones in normal and dysmorphic sacra. J Orthop Trauma 24(10):622–629. doi:10.1097/BOT.0b013e3181cf0404
Moed BR, Whiting DR (2010) Locked transsacral screw fixation of bilateral injuries of the posterior pelvic ring: initial clinical series. J Orthop Trauma 24(10):616–621. doi:10.1097/BOT.0b013e3181df97eb
Beaule PE, Antoniades J, Matta JM (2006) Trans-sacral fixation for failed posterior fixation of the pelvic ring. Arch Orthop Trauma Surg 126(1):49–52. doi:10.1007/s00402-005-0069-2
Gras F, Hillmann S, Rausch S, Klos K, Hofmann GO, Marintschev I (2015) Biomorphometric analysis of ilio-sacro-iliacal corridors for an intra-osseous implant to fix posterior pelvic ring fractures. J Orthop Res: Off Publ Orthop Res Soc 33(2):254–260. doi:10.1002/jor.22754
Denis F, Davis S, Comfort T (1988) Sacral fractures: an important problem. Retrospective analysis of 236 cases. Clin Orthop Relat Res 227:67–81
Mullis BH, Sagi HC (2008) Minimum 1-year follow-up for patients with vertical shear sacroiliac joint dislocations treated with iliosacral screws: does joint ankylosis or anatomic reduction contribute to functional outcome? J Orthop Trauma 22(5):293–298. doi:10.1097/BOT.0b013e31816b6b4e
Dujardin FH, Hossenbaccus M, Duparc F, Biga N, Thomine JM (1998) Long-term functional prognosis of posterior injuries in high-energy pelvic disruption. J Orthop Trauma 12(3):145–150, discussion 150–141
McLaren AC, Rorabeck CH, Halpenny J (1990) Long-term pain and disability in relation to residual deformity after displaced pelvic ring fractures. Can J Surg J Can Chir 33(6):492–494
Nepola JV, Trenhaile SW, Miranda MA, Butterfield SL, Fredericks DC, Riemer BL (1999) Vertical shear injuries: is there a relationship between residual displacement and functional outcome? J Trauma 46(6):1024–1029, discussion 1029–1030
Heiner AD (2008) Structural properties of fourth-generation composite femurs and tibias. J Biomech 41(15):3282–3284. doi:10.1016/j.jbiomech.2008.08.013
van Zwienen CM, van den Bosch EW, Snijders CJ, Kleinrensink GJ, van Vugt AB (2004) Biomechanical comparison of sacroiliac screw techniques for unstable pelvic ring fractures. J Orthop Trauma 18(9):589–595
Clements JP, Moriaty N, Chesser TJ, Ward AJ, Cunningham JL (2008) Determination of pelvic ring stability: a new technique using a composite hemi-pelvis. Proc Inst Mech Eng H J Eng Med 222(5):611–616
Acknowledgments
The authors are not compensated and there are no other institutional subsidies, corporate affiliations, or funding sources supporting this work unless clearly documented and disclosed. This investigation was performed with the assistance of the AO Foundation via the AOTRAUMA Network (Grant No.: AR2013_10).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Additional information
Gaston Camino Willhuber and Ivan Zderic contributed equally to this work.
Rights and permissions
About this article
Cite this article
Camino Willhuber, G., Zderic, I., Gras, F. et al. Analysis of sacro-iliac joint screw fixation: does quality of reduction and screw orientation influence joint stability? A biomechanical study. International Orthopaedics (SICOT) 40, 1537–1543 (2016). https://doi.org/10.1007/s00264-015-3007-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-015-3007-0