Abstract
Purpose
Surgery for spinal metastasis is often associated with significant morbidity. Despite a number of preoperative scoring systems/scales and identified variables that have been reported to predict complication risk, clinical studies that directly evaluate this issue using multivariate analysis are scarce. The goal of our study was to assess independent predictors of complication after surgery for spinal metastasis.
Methods
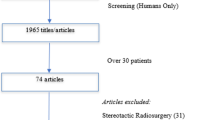
We queried electronic medical records to identify a consecutive population of adult patients who underwent surgery for spinal metastasis for the period June 2005 through June 2011. Utilizing multivariate logistic regression, we assessed independent predictors of perioperative and postoperative adverse events.
Results
A total of 106 patients were included in the final analysis. Overall complication rate was 21.7 %. Independent predictors for higher rates of complication were age greater than 40 years [40–65 years had odds ratio (OR) 1.91, 95 % confidence interval (CI) 1.02–16.78 and >65 years had OR 5.17, 95 % CI 1.54–29.81] and metastatic lesions involving three or more contiguous levels of the spine (OR 2.76, 95 % CI 1.09–9.61).
Conclusions
Patients older than 40 years or patients who have metastatic lesions involving three or more contiguous vertebral levels appear to be at higher risk for complication. Patients older than 65 years have the greatest likelihood of complication.
Similar content being viewed by others
References
Finkelstein JA, Zaveri G, Wai E, Vidmar M, Kreder H, Chow E (2003) A population-based study of surgery for spinal metastases. Survival rates and complications. J Bone Jt Surg Br 85:1045–1050
Onimus M, Papin P, Gangloff S (1996) Results of surgical treatment of spinal thoracic and lumbar metastases. Eur Spine J 5:407–411
Wibmer C, Leithner A, Hofmann G, Clar H, Kapitan M, Berghold A, Windhager R (2011) Survival analysis of 254 patients after manifestation of spinal metastases: evaluation of seven preoperative scoring systems. Spine (Phila Pa 1976) 36:1977–1986
Arrigo RT, Kalanithi P, Cheng I, Alamin T, Carragee EJ, Mindea SA, Park J, Boakye M (2011) Predictors of survival after surgical treatment of spinal metastasis. Neurosurgery 68:674–681
Quan GM, Vital JM, Aurouer N, Obeid I, Palussiere J, Diallo A, Pointillart V (2011) Surgery improves pain, function and quality of life in patients with spinal metastases: a prospective study on 118 patients. Eur Spine J 20:1970–1978
Williams BJ, Fox BD, Sciubba DM, Suki D, Tu SM, Kuban D, Gokaslan ZL, Rhines LD, Rao G (2009) Surgical management of prostate cancer metastatic to the spine. J Neurosurg Spine 10:414–422
Wise JJ, Fischgrund JS, Herkowitz HN, Montgomery D, Kurz LT (1999) Complication, survival rates, and risk factors of surgery for metastatic disease of the spine. Spine (Phila Pa 1976) 24:1943–1951
Arrigo RT, Kalanithi P, Cheng I, Alamin T, Carragee EJ, Mindea SA, Boakye M, Park J (2011) Charlson score is a robust predictor of 30-day complications following spinal metastasis surgery. Spine (Phila Pa 1976) 36:E1274–E1280
Demura S, Kawahara N, Murakami H, Nambu K, Kato S, Yoshioka K, Okayama T, Tomita K (2009) Surgical site infection in spinal metastasis: risk factors and countermeasures. Spine (Phila Pa 1976) 34:635–639
Shehadi JA, Sciubba DM, Suk I, Suki D, Maldaun MV, McCutcheon IE, Nader R, Theriault R, Rhines LD, Gokaslan ZL (2007) Surgical treatment strategies and outcome in patients with breast cancer metastatic to the spine: a review of 87 patients. Eur Spine J 16:1179–1192
Seo SH, Hur H, An CW, Yi X, Kim JY, Han SU, Cho YK (2011) Operative risk factors in gastric cancer surgery for elderly patients. J Gastric Cancer 11:116–121
Schoenfeld AJ, Ochoa LM, Bader JO, Belmont PJ Jr (2011) Risk factors for immediate postoperative complications and mortality following spine surgery: a study of 3475 patients from the national surgical quality improvement program. J Bone Jt Surg Am 93:1577–1582
Cloyd JM, Acosta FL Jr, Cloyd C, Ames CP (2010) Effects of age on perioperative complications of extensive multilevel thoracolumbar spinal fusion surgery. J Neurosurg Spine 12:402–408
Lau D, El-Sayed AM, Ziewacz JE, Jayachandran P, Huq FS, Zamora-Berridi GJ, Davis MC, Sullivan SE (2012) Postoperative outcomes following closed head injury and craniotomy for evacuation of hematoma in patients older than 80 years. J Neurosurg 116:234–245
Lans TE, van der Pol C, Wouters MW, Schmitz PI, van Geel AN (2009) Complications in wound healing after chest wall resection in cancer patients; a multivariate analysis of 220 patients. J Thorac Oncol 4:639–643
Payne WG, Naidu DK, Wheeler CK, Barkoe D, Mentis M, Salas RE, Smith DJ Jr, Robson MC (2008) Wound healing in patients with cancer. Eplasty 8:e9
Byrne M, Reynolds JV, O’Donnell JS, Keogan M, White B, Murphy S, Maher SG, Pidgeon GP (2010) Long-term activation of the pro-coagulant response after neoadjuvant chemoradiation and major cancer surgery. Br J Cancer 102:73–79
Huppert J, Beaurain J, Steib JP, Bernard P, Dufour T, Hovorka I, Stecken J, Dam-Hieu P, Fuentes JM, Vital JM, Vila T, Aubourg L (2011) Comparison between single- and multi-level patients: clinical and radiological outcomes 2 years after cervical disc replacement. Eur Spine J 20:1417–1426
Lettice JJ, Kula TA, Derby R, Kim BJ, Lee SH, Seo KS (2005) Does the number of levels affect lumbar fusion outcome? Spine (Phila Pa 1976) 30:675–681
Lawrence VA, Hilsenbeck SG, Mulrow CD, Dhanda R, Sapp J, Page CP (1995) Incidence and hospital stay for cardiac and pulmonary complications after abdominal surgery. J Gen Intern Med 10:671–678
Polanczyk CA, Marcantonio E, Goldman L, Rohde LE, Orav J, Mangione CM, Lee TH (2001) Impact of age on perioperative complications and length of stay in patients undergoing noncardiac surgery. Ann Intern Med 134:637–643
Falicov A, Fisher CG, Sparkes J, Boyd MC, Wing PC, Dvorak MF (2006) Impact of surgical intervention on quality of life in patients with spinal metastases. Spine (Phila Pa 1976) 31:2849–2856
Fujibayashi S, Neo M, Miyaki K, Nakayama T, Nakamura T (2010) The value of palliative surgery for metastatic spinal disease: satisfaction of patients and their families. Spine J 10:42–49
Conflict of interest
Dr. Park is a consultant for Globus Medical and DePuy Spine and has received an honorarium from Medtronic in the past year. Dr. La Marca is a consultant for Globus Medical, Biomet, Lanx, and Stryker. None of the authors report a conflict of interest associated with the contents of this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lau, D., Leach, M.R., Than, K.D. et al. Independent predictors of complication following surgery for spinal metastasis. Eur Spine J 22, 1402–1407 (2013). https://doi.org/10.1007/s00586-013-2706-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-013-2706-8