Abstract
Purpose
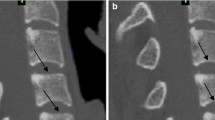
Construct subsidence is a relatively common complication following anterior cervical fusion. Its occurrence has been revealed to be closely related to endplate-implant contact interface. But current literature focusing on the anatomy of cervical endplate is very scarce. The purpose of this morphometric study was to analyse the sagittal geometry, especially the concavity and slope, of vertebral endplates from C3 to C7 by employing data from CT scans.
Methods
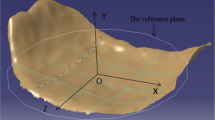
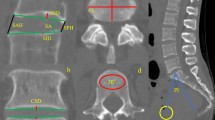
Reformatted CT scans of 97 individuals were analyzed and endplate concavity depth, endplate concavity apex location, as well as endplate slope were measured in midsagittal plane. Those specific parameters were compared among different age and gender groups. Meanwhile, comparison between superior and inferior endplate of each vertebra was also performed.
Results
Age and gender did not influence endplate concavity depth, endplate concavity apex location, or endplate slope significantly (P > 0.05). Endplate concavity depths of superior endplates (range 0.9–1.2 mm) were significantly smaller than those of inferior endplates (range 2.1–2.7 mm). Endplate concavity apex was always located in the posterior half of the endplate, with the superior one ranged from 56 to 67 % and the inferior one 52 to 57 %. Average endplate slopes of superior endplates were between 4.5° and 9.0°, and average inferior endplate slopes ranged from 4.5° to 7.5°. Among all measured segments, C5 had the largest endplate slope values, while C7 the least.
Conclusions
Superior endplate is more flat than its inferior counterpart in middle and lower cervical spine, and the concavity apex is always located in the posterior half of the endplate. Endplate slope is correlated with cervical curvature, greater slope implying more significant lordosis. These sagittal endplate geometrical parameters should be taken into consideration when investigating implant subsidence following anterior cervical fusion.



Similar content being viewed by others
References
Bohlman HH, Emery SE, Goodfellow DB, Jones PK (1993) Robinson anterior cervical discectomy and arthrodesis for cervical radiculopathy. Long-term follow-up of one hundred and twenty-two patients. J Bone Joint Surg Am 75:1298–1307
Emery SE, Bolesta MJ, Banks MA, Jones PK (1994) Robinson anterior cervical fusion comparison of the standard and modified techniques. Spine 19:660–663
van Jonbergen HP, Spruit M, Anderson PG, Pavlov PW (2005) Anterior cervical interbody fusion with a titanium box cage: early radiological assessment of fusion and subsidence. Spine J 5:645–649 discussion 649
Kao FC, Niu CC, Chen LH, Lai PL, Chen WJ (2005) Maintenance of interbody space in one- and two-level anterior cervical interbody fusion: comparison of the effectiveness of autograft, allograft, and cage. Clin Orthopaed Relat Res 430:108–116
Grob D, Daehn S, Mannion AF (2005) Titanium mesh cages (TMC) in spine surgery. Eur Spine J 14:211–221
Chou YC, Chen DC, Hsieh WA, Chen WF, Yen PS, Harnod T, Chiou TL, Chang YL, Su CF, Lin SZ, Chen SY (2008) Efficacy of anterior cervical fusion: comparison of titanium cages, polyetheretherketone (PEEK) cages and autogenous bone grafts. J Clin Neurosci 15:1240–1245
Niu CC, Liao JC, Chen WJ, Chen LH (2012) Outcomes of interbody fusion cages used in 1 and 2-levels anterior cervical discectomy and fusion: titanium cages versus polyetheretherketone (PEEK) cages. J Spinal Disord Tech 23:310–316
Barsa P, Suchomel P (2007) Factors affecting sagittal malalignment due to cage subsidence in standalone cage assisted anterior cervical fusion. Eur Spine J 16:1395–1400
Cabraja M, Oezdemir S, Koeppen D, Kroppenstedt S (2012) Anterior cervical discectomy and fusion: comparison of titanium and polyetheretherketone cages. BMC Musculoskelet Disord 13:172
Buttermann GR, Beaubien BP, Freeman AL, Stoll JE, Chappuis JL (2009) Interbody device endplate engagement effects on motion segment biomechanics. Spine J 9:564–573
Kim MK, Kwak DS, Park CK, Park SH, Oh SM, Lee SW, Han SH (2007) Quantitative anatomy of the endplate of the middle and lower cervical vertebrae in Koreans. Spine 32:E376–E381
Tan SH, Teo EC, Chua HC (2004) Quantitative three-dimensional anatomy of cervical, thoracic and lumbar vertebrae of Chinese Singaporeans. Eur Spine J 13:137–146
Van Ooij A, Oner F, Verbout A (2003) Complications of artificial disc replacement: a report of 27 patients with the SB Charite disc. J Spinal Disord Tech 16:369–383
Edwards WT, Zheng Y, Ferrara LA, Yuan HA (2001) Structural features and thickness of the vertebral cortex in the thoracolumbar spine. Spine 26:218–225
Lakshmanan P, Purushothaman B, Dvorak V, Schratt W, Thambiraj S, Boszczyk M (2012) Sagittal endplate morphology of the lower lumbar spine. Eur Spine J Suppl 2:S160–S164
Chen H, Jiang D, Ou Y, Zhong J, Lv F (2011) Geometry of thoracolumbar vertebral endplates of the human spine. Eur Spine J 20:1814–1820
van der Houwen EB, Baron P, Veldhuizen AG, Burgerhof JG, van Ooijen PM, Verkerke GJ (2010) Geometry of the intervertebral volume and vertebral endplates of the human spine. Ann Biomed Eng 38:33–40
Rockoff SD, Sweet E, Bleustein J (1969) The relative contribution of trabecular and cortical bone to the strength of human lumbar vertebrae. Calcif Tissue Res 3:163–175
Lowe TG, Hashim S, Wilson LA, O’Brien MF, Smith DA, Diekmann MJ, Trommeter J (2004) A biomechanical study of regional endplate strength and cage morphology as it relates to structural interbody support. Spine 29:2389–2394
Twomey LT, Taylor JR (1987) Age changes in lumbar vertebrae and intervertebral discs. Clin Orthop Relat Res 224:97–104
Ferguson SJ, Steffen T (2003) Biomechanics of the aging spine. Eur Spine J Suppl 2:S97–S103
Miao S, Sha GZ, Wang YD, Yan LQ, Song LY, Guo Z, Fan L, Shao L (2008) Imageology change of degenerative cartilage endplate to different degree and its clinical significance. Zhongguo Gu Shang 21:414–417
He X, Liang A, Gao W, Peng Y, Zhang L, Liang G, Huang D (2012) The relationship between concave angle of vertebral endplate and lumbar intervertebral disc degeneration. Spine 37:E1068–E1073
Buttermann GR, Freeman AL, Beaubien BP (2010) In vitro biomechanics of an expandable vertebral body replacement with self-adjusting end plates. Spine J 10:1024–1031
Pflugmacher R, Schleicher P, Schaefer J, Scholz M, Ludwig K, Khodadadyan-Klostermann C, Haas NP, Kandziora F (2004) Biomechanical comparison of expandable cages for vertebral body replacement in the thoracolumbar spine. Spine 29:1413–1419
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, H., Zhong, J., Tan, J. et al. Sagittal geometry of the middle and lower cervical endplates. Eur Spine J 22, 1570–1575 (2013). https://doi.org/10.1007/s00586-013-2791-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-013-2791-8