Abstract
Study design
A cross-sectional study of the data retrospectively collected by chart review.
Objectives
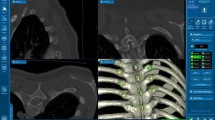
This study aimed to clarify screw perforation features in 129 consecutive patients treated with computer-assisted cervical pedicle screw (CPS) insertion and to determine important considerations for computer-assisted CPS insertion.
Summary of background data
CPS fixation has been criticized for the potential risk of serious injury to neurovascular structures. To avoid such serious risks, computed tomography (CT)-based navigation has been used during CPS insertion, but screw perforation can occur even with the use of a navigation system.
Methods
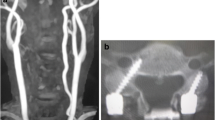
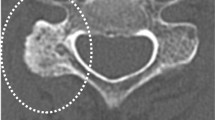
The records of 129 consecutive patients who underwent cervical (C2–C7) pedicle screw insertion using a CT-based navigation system from September 1997 to August 2013 were reviewed. Postoperative CT images were used to evaluate the accuracy of screw placement. The screw insertion status was classified as grade 1 (no perforation), indicating that the screw was accurately inserted in pedicle; grade 2 (minor perforation), indicating perforation of less than 50 % of the screw diameter; and grade 3 (major perforation), indicating perforation of 50 % or more of the screw diameter. We analyzed the direction and rate of screw perforation according to the vertebral level.
Results
The rate of grade 3 pedicle screw perforations was 6.7 % (39/579), whereas the combined rate of grades 2 and 3 perforations was 20.0 % (116/579). No clinically significant complications, such as vertebral artery injury, spinal cord injury, or nerve root injury, were caused by the screw perforations. Of the screws showing grade 3 perforation, 30.8 % screws were medially perforated and 69.2 % screws were laterally perforated. Of the screws showing grades 2 and 3 perforation, 21.6 % screws were medially perforated and 78.4 % screws were laterally perforated. Furthermore, we evaluated screw perforation rates according to the vertebral level. Grade 3 pedicle screw perforation occurred in 6.1 % of C2 screws; 7.5 % of C3 screws; 13.0 % of C4 screws; 6.5 % of C5 screws; 3.2 % of C6 screws; and 4.0 % of C7 screws. Grades 2 and 3 pedicle screw perforations occurred in 12.1 % of C2 screws, 22.6 % of C3 screws, 31.5 % of C4 screws, 22.2 % of C5 screws, 14.4 % of C6 screws, and 12.1 % of C7 screws. C3–5 screw perforation rate was significantly higher than C6–7 (p = 0.0024).
Conclusions
Careful insertion of pedicle screws is necessary, especially at C3 to C5, even when using a CT-based navigation system. Pedicle screws tend to be laterally perforated.


Similar content being viewed by others
References
Abumi K, Itoh H, Taneichi H, Kaneda K (1994) Transpedicular screw fixation for traumatic lesions of the middle and lower cervical spine: description of the techniques and preliminary report. J Spinal Disord 7:19–28
Abumi K, Kaneda K, Shono Y, Fujiyama M (1999) One-stage posterior decompression and reconstruction of the cervical spine by using pedicle screw fixation systems. J Neurosurg 90:19–26
Anderson PA, Henley MB, Grady MS, Montesano PX, Winn HR (1991) Posterior cervical arthrodesis with AO reconstruction plates and bone graft. Spine 16:S72–S79
Chazono M, Soshi S, Inoue T, Kida Y, Ushiku C (2006) Anatomical considerations for cervical pedicle screw insertion: the use of multiplanar computerized tomography reconstruction measurements. J Neurosurg Spine 4:472–477
Ishikawa Y, Kanemura T, Yoshida G, Ito Z, Muramoto A, Ohno S (2010) Clinical accuracy of three-dimensional fluoroscopy-based computer-assisted cervical pedicle screw placement: a retrospective comparative study of conventional versus computer-assisted cervical pedicle screw placement. J Neurosurg Spine 13:606–611
Janneret B, Gebhard JS, Magerl F (1994) Transpedicular screw fixation of articular mass fracture separation: results of an anatomical study and operative technique. J Spinal Disord 7:222–229
Jo DJ, Seo EM, Kim KT, Kim SM, Lee SH (2012) Cervical pedicle screw insertion using the technique with direct exposure of the pedicle by laminoforaminotomy. J Korean Neurosurg Soc 52:459–465
Johnston TL, Karaikovic EE, Lautenschlager EP, Marucu D (2006) Cervical pedicle screws vs. lateral mass screws: uniplanar fatigue analysis and residual pullout strengths. Spine J 6:667–672
Jones EI, Heller JG, Silcox DH, Hutton WC (1997) Cervical pedicle screws versus lateral mass screws: anatomic feasibility and biomechanical comparison. Spine 22:977–982
Karaikovic EE, Kunakornsawat S, Daubs MD, Madsen TW, Gaines RW Jr (2000) Surgical anatomy of the cervical pedicles: landmarks for posterior cervical pedicle entrance localization. J Spinal Disord 13:63–72
Kotani Y, Abumi K, Ito M, Minami A (2003) Improved accuracy of computer-assisted cervical pedicle screw insertion. J Neurosurg 99(3 Suppl):257–263
Kotil K, Sengoz A, Savas Y (2011) Cervical transpedicular fixation aided by biplanar fluoroscopy. J Orthop Surg (Hong Kong) 19:326–330
Ogihara N, Takahashi J, Hirabayashi H, Hashidate H, Kato H (2010) Long-term results of computer-assisted posterior occipitocervical reconstruction. World Neurosurg 73:722–728
Onibokun A, Khoo LT, Bistazzoni S, Chen NF, Sassi M (2009) Anatomical considerations for cervical pedicle screw insertion: the use of multiplanar computerized tomography measurements in 122 consecutive clinical cases. Spine J 9:729–734
Rhee JM, Kraiwattanapong C, Hutton WC (2005) A comparison of pedicle and lateral mass screw construct stiffnesses at the cervicothoracic junction: biomechanical study. Spine 30:E636–E640
Takahashi J, Hirabayashi H, Hashidate H, Ogihara N, Kato H (2010) Accuracy of multilevel registration in image-guided pedicle screw insertion for adolescent idiopathic scoliosis. Spine 35(3):347–352
Tauchi R, Imagama S, Sakai Y, Ito Z, Ando K, Muramoto A, Matsui H, Matsumoto T, Ishiguro N (2013) The correlation between cervical range of motion and misplacement of cervical pedicle screws during cervical posterior spinal fixation surgery using a CT-based navigation system. Eur Spine J 22:1504–1508
Tian NF, Xu HZ (2009) Image-guided pedicle screw insertion accuracy: a meta-analysis. Int Orthop 33:895–903
Wang Y, Xie J, Yang Z, Zhao Z, Zhang Y, Li T, Liu L (2013) Computed tomography assessment of lateral pedicle wall perforation by free-hand subaxial cervical pedicle screw placement. Arch Orthop Trauma Surg 133:901–909
Yukawa Y, Kato F, Ito K, Horie Y, Hida T, Nakashima H, Machino M (2009) Placement and complications of cervical pedicle screws in 144 cervical trauma patients using pedicle axis view techniques by fluoroscope. Eur Spine J 18:1293–1299
Conflict of interest
None of the authors of this manuscript received any type of support, benefits, or funding from a commercial party related directly or indirectly to the subject of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Uehara, M., Takahashi, J., Ikegami, S. et al. Screw perforation features in 129 consecutive patients performed computer-guided cervical pedicle screw insertion. Eur Spine J 23, 2189–2195 (2014). https://doi.org/10.1007/s00586-014-3502-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3502-9