Abstract
Purpose
To assess the cost–utility and perioperative costs of minimally invasive transforaminal lumbar interbody fusion (MI-TLIF) versus open-TLIF for degenerative lumbar pathologies.
Methods
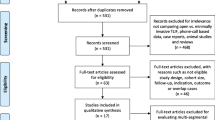
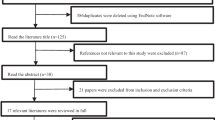
Relevant articles were identified from six electronic databases. Predefined end points were extracted and meta-analysis conducted from the identified studies.
Results
For each study, the direct hospital cost for MI-TLIF was found to be less than that of open-TLIF. When these outcomes were pooled, direct hospital costs were found to be significantly lower in the MI-TLIF group [weighted mean difference (WMD), −$2820; I 2 = 61 %; P < 0.00001]. MI-TLIF was also associated with shorter hospitalization (WMD, 0.99; 95 % CI −1.81, −0.17; I 2 = 96 %; P = 0.02), trend toward reduced complications (relative risk 0.53; 95 % CI 0.23, 1.06; I 2 = 0 %; P = 0.07), and reduced blood loss (WMD, −246.40 mL; I 2 = 98 %; P = 0.003), but was not associated with a significant difference in operation time (WMD, −67.05; 95 % CI −169.44, 35.35; I 2 = 100 %; P = 0.20).
Conclusions
From the limited evidence, the available data suggest a trend of significantly reduced perioperative costs, length of stay, and blood loss for minimally invasive compared with open surgical approaches for TLIF. MI-TLIF may represent an opportunity for optimal utilization and allocation of health-care resources from both a hospital and societal perspective.




Similar content being viewed by others
References
Harms J, Rolinger H (1982) A one-stager procedure in operative treatment of spondylolistheses: dorsal traction-reposition and anterior fusion (author’s transl). Z Orthop Ihre Grenzgeb 120:343–347. doi:10.1055/s-2008-1051624
Hackenberg L, Halm H, Bullmann V, Vieth V, Schneider M, Liljenqvist U (2005) Transforaminal lumbar interbody fusion: a safe technique with satisfactory three to five year results. Eur Spine J 14:551–558. doi:10.1007/s00586-004-0830-1
Archavlis E, Carvi y Nievas M (2013) Comparison of minimally invasive fusion and instrumentation versus open surgery for severe stenotic spondylolisthesis with high-grade facet joint osteoarthritis. Eur Spine J 22:1731–1740. doi:10.1007/s00586-013-2732-6
Brodano GB, Martikos K, Lolli F, Gasbarrini A, Cioni A, Bandiera S, Di Silvestre M, Boriani S, Greggi T (2013) Transforaminal lumbar interbody fusion in degenerative disc disease and spondylolisthesis grade i: minimally invasive versus open surgery. J Spinal Disord Tech. doi:10.1097/BSD.0000000000000034
Assaker R (2004) Minimal access spinal technologies: state-of-the-art, indications, and techniques. Joint Bone Spine 71:459–469. doi:10.1016/j.jbspin.2004.08.006
Gu G, Zhang H, Fan G, He S, Cai X, Shen X, Guan X, Zhou X (2014) Comparison of minimally invasive versus open transforaminal lumbar interbody fusion in two-level degenerative lumbar disease. Int Orthop 38:817–824. doi:10.1007/s00264-013-2169-x
Phan K, Rao PJ, Kam AC, Mobbs RJ (2015) Minimally invasive versus open transforaminal lumbar interbody fusion for treatment of degenerative lumbar disease: systematic review and meta-analysis. Eur Spine J 24:1017–1030. doi:10.1007/s00586-015-3903-4
Tian NF, Wu YS, Zhang XL, Xu HZ, Chi YL, Mao FM (2013) Minimally invasive versus open transforaminal lumbar interbody fusion: a meta-analysis based on the current evidence. Eur Spine J 22:1741–1749. doi:10.1007/s00586-013-2747-z
Lubelski D, Mihalovich KE, Skelly AC, Fehlings MG, Harrop JS, Mummaneni PV, Wang MY, Steinmetz MP (2014) Is minimal access spine surgery more cost-effective than conventional spine surgery? Spine 39:S65–S74. doi:10.1097/brs.0000000000000571
Al-Khouja LT, Baron EM, Johnson JP, Kim TT, Drazin D (2014) Cost-effectiveness analysis in minimally invasive spine surgery. Neurosurg Focus 36:E4. doi:10.3171/2014.4.focus1449
Lucio JC, Vanconia RB, Deluzio KJ, Lehmen JA, Rodgers JA, Rodgers W (2012) Economics of less invasive spinal surgery: an analysis of hospital cost differences between open and minimally invasive instrumented spinal fusion procedures during the perioperative period. Risk Manag Healthc Policy 5:65–74. doi:10.2147/rmhp.s30974
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 151(264–269):W264
Shea BJ, Grimshaw JM, Wells GA, Boers M, Andersson N, Hamel C, Porter AC, Tugwell P, Moher D, Bouter LM (2007) Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Med Res Methodol 7:10. doi:10.1186/1471-2288-7-10
Phan K, Tian DH, Cao C, Black D, Yan TD (2015) Systematic review and meta-analysis: techniques and a guide for the academic surgeon. Ann Cardiothorac Surg 4:112–122. doi:10.3978/j.issn.2225-319X.2015.02.04
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA 283:2008–2012
Ostelo RW, Deyo RA, Stratford P, Waddell G, Croft P, Von Korff M, Bouter LM, de Vet HC (2008) Interpreting change scores for pain and functional status in low back pain: towards international consensus regarding minimal important change. Spine 33:90–94. doi:10.1097/BRS.0b013e31815e3a10
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56:455–463
Sulaiman WA, Singh M (2014) Minimally invasive versus open transforaminal lumbar interbody fusion for degenerative spondylolisthesis grades 1–2: patient-reported clinical outcomes and cost-utility analysis. Ochsner J 14:32–37
Singh K, Nandyala SV, Marquez-Lara A, Fineberg SJ, Oglesby M, Pelton MA, Andersson GB, Isayeva D, Jegier BJ, Phillips FM (2014) A perioperative cost analysis comparing single-level minimally invasive and open transforaminal lumbar interbody fusion. Spine J 14:1694–1701. doi:10.1016/j.spinee.2013.10.053
Parker SL, Adogwa O, Bydon A, Cheng J, McGirt MJ (2012) Cost-effectiveness of minimally invasive versus open transforaminal lumbar interbody fusion for degenerative spondylolisthesis associated low-back and leg pain over two years. World Neurosurg 78:178–184. doi:10.1016/j.wneu.2011.09.013
Parker SL, Mendenhall SK, Shau DN, Zuckerman SL, Godil SS, Cheng JS, McGirt MJ (2014) Minimally invasive versus open transforaminal lumbar interbody fusion for degenerative spondylolisthesis: comparative effectiveness and cost-utility analysis. World Neurosurg 82:230–238. doi:10.1016/j.wneu.2013.01.041
Pelton MA, Phillips FM, Singh K (2012) A comparison of perioperative costs and outcomes in patients with and without workers’ compensation claims treated with minimally invasive or open transforaminal lumbar interbody fusion. Spine 37:1914–1919. doi:10.1097/BRS.0b013e318257d490
Rampersaud YR, Gray R, Lewis SJ, Massicotte EM, Fehlings MG (2011) Cost-utility analysis of posterior minimally invasive fusion compared with conventional open fusion for lumbar spondylolisthesis. SAS J 5:29–35. doi:10.1016/j.esas.2011.02.001
Wang MY, Lerner J, Lesko J, McGirt MJ (2012) Acute hospital costs after minimally invasive versus open lumbar interbody fusion: data from a US national database with 6106 patients. J Spinal Disord Tech 25:324–328. doi:10.1097/BSD.0b013e318220be32
Wang MY, Cummock MD, Yu Y, Trivedi RA (2010) An analysis of the differences in the acute hospitalization charges following minimally invasive versus open posterior lumbar interbody fusion. J Neurosurg Spine 12:694–699. doi:10.3171/2009.12.SPINE09621
McGirt MJ, Parker SL, Lerner J, Engelhart L, Knight T, Wang MY (2011) Comparative analysis of perioperative surgical site infection after minimally invasive versus open posterior/transforaminal lumbar interbody fusion: analysis of hospital billing and discharge data from 5170 patients. J Neurosurg Spine 14:771–778. doi:10.3171/2011.1.SPINE10571
Parker SL, Adogwa O, Witham TF, Aaronson OS, Cheng J, McGirt MJ (2011) Post-operative infection after minimally invasive versus open transforaminal lumbar interbody fusion (TLIF): literature review and cost analysis. MIN 54:33–37. doi:10.1055/s-0030-1269904
Dagenais S, Caro J, Haldeman S (2008) A systematic review of low back pain cost of illness studies in the United States and internationally. Spine J 8:8–20. doi:10.1016/j.spinee.2007.10.005
Davis MA, Onega T, Weeks WB, Lurie JD (2012) Where the United States spends its spine dollars: expenditures on different ambulatory services for the management of back and neck conditions. Spine 37:1693–1701. doi:10.1097/BRS.0b013e3182541f45
Martin BI, Turner JA, Mirza SK, Lee MJ, Comstock BA, Deyo RA (2009) Trends in health care expenditures, utilization, and health status among US adults with spine problems, 1997–2006. Spine 34:2077–2084. doi:10.1097/BRS.0b013e3181b1fad1
Phan K, Thayaparan GK, Mobbs RJ (2015) Anterior lumbar interbody fusion versus transforaminal lumbar interbody fusion—systematic review and meta-analysis. Br J Neurosurg 12:1–7. doi:10.3109/02688697.2015.1036838
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None declared.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Phan, K., Hogan, J.A. & Mobbs, R.J. Cost–utility of minimally invasive versus open transforaminal lumbar interbody fusion: systematic review and economic evaluation. Eur Spine J 24, 2503–2513 (2015). https://doi.org/10.1007/s00586-015-4126-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4126-4