Abstract
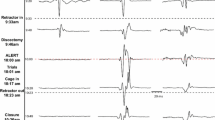
Injury to the lumbosacral (LS) plexus is a well-described complication after lateral retroperitoneal transpsoas approaches to the spine. The prognosis for functional recovery after lumbosacral plexopathy or femoral/obturator neuropathy is unclear. We designed a retrospective case-control study with patients undergoing one-level lateral retroperitoneal transpsoas lumbar interbody fusion (LLIF) between January 2011 and June 2016 to correlate electrodiagnostic assessments (EDX) to physiologic concepts of nerve injury and reinnervation, and attempt to build a timeline for patient evaluation and recovery. Cases with post-operative obturator or femoral neuropathy were identified. Post-operative MRI, nerve conduction studies (NCS), electromyography (EMG), and physical examinations were performed at intervals to assess clinical and electrophysiologic recovery of function. Two hundred thirty patients underwent LLIF. Six patients (2.6%) suffered severe femoral or femoral/obturator neuropathy. Five patients (2.2%) had immediate post-operative weakness. One of the six patients developed delayed weakness due to a retroperitoneal hematoma. Five out of six patients (83%) demonstrated EDX findings at 6 weeks consistent with axonotmesis. All patients improved to at least MRC 4/5 within 12 months of injury. In conclusion, neurapraxia is the most common LS plexus injury, and complete recovery is expected after 3 months. Most severe nerve injuries are a combination of neurapraxia and variable degrees of axonotmesis. EDX performed at 6 weeks and 3, 6, and 9 months provides prognostic information for recovery. In severe injuries of proximal femoral and obturator nerves, observation of proximal to distal progression of small-amplitude, short-duration (SASD) motor unit potentials may be the most significant prognostic indicator.


Similar content being viewed by others
References
Ahmadian A, Deukmedjian AR, Abel N, Dakwar E, Uribe JS (2013) Analysis of lumbar plexopathies and nerve injury after lateral retroperitoneal transpsoas approach: diagnostic standardization. J Neurosurg Spine. 18(3):289–297
Cummock MD, Vanni S, Levi AD, Yu Y, Wang MY (2011) An analysis of postoperative thigh symptoms after minimally invasive transpsoas lumbar interbody fusion. J Neurosurg Spine. 15(1):11–18
Cahill KS, Martinez JL, Wang MY, Vanni S, Levi AD (2012) Motor nerve injuries following the minimally invasive lateral transpsoas approach. J Neurosurg Spine. 17(3):227–231
Stewart JD (2000) Focal Peripheral Neuropathies. Lippincott Williams & Wilkins
Ozgur BM, Aryan HE, Pimenta L, Taylor WR (2006) Extreme lateral interbody fusion (XLIF): a novel surgical technique for anterior lumbar interbody fusion. Spine J 6(4):435–443
Sunderland S (1990) The anatomy and physiology of nerve injury. Muscle Nerve 13(9):771–784
Patel S (2015) Chapter 34 - Human dermatomes A2 - Tubbs, R. Shane. In: Rizk E, Shoja MM, Loukas M, Barbaro N, Spinner RJ (eds) Nerves and nerve injuries. Academic Press, San Diego, pp 477–483
Lykissas MG, Aichmair A, Hughes AP, Sama AA, Lebl DR, Taher F, Du JY, Cammisa FP, Girardi FP (2014) Nerve injury after lateral lumbar interbody fusion: a review of 919 treated levels with identification of risk factors. Spine J 14(5):749–758
Muheremu A, Ao Q (2015) Past, present, and future of nerve conduits in the treatment of peripheral nerve injury. BioMed Res Int 2015:237507
Uribe JS, Isaacs RE, Youssef JA, Khajavi K, Balzer JR, Kanter AS, Kuelling FA, Peterson MD (2015) Can triggered electromyography monitoring throughout retraction predict postoperative symptomatic neuropraxia after XLIF? Results from a prospective multicenter trial. Eur Spine J 24(Suppl 3):378–385
Uribe JS, Arredondo N, Dakwar E, Vale FL (2010) Defining the safe working zones using the minimally invasive lateral retroperitoneal transpsoas approach: an anatomical study. J Neurosurg Spine 13(2):260–266
Boyd KU, Nimigan AS, Mackinnon SE (2011) Nerve reconstruction in the hand and upper extremity. Clin Plast Surg 38(4):643–660
Isaacs RE, Hyde J, Goodrich JA, Rodgers WB, Phillips FM (2010) A prospective, nonrandomized, multicenter evaluation of extreme lateral interbody fusion for the treatment of adult degenerative scoliosis: perioperative outcomes and complications. Spine 35(26 Suppl):S322–S330
Pumberger M, Hughes AP, Huang RR, Sama AA, Cammisa FP, Girardi FP (2012) Neurologic deficit following lateral lumbar interbody fusion. Eur Spine J 21(6):1192–1199
Kuntzer T, van Melle G, Regli F (1997) Clinical and prognostic features in unilateral femoral neuropathies. Muscle Nerve 20(2):205–211
Campbell AA, Eckhauser FE, Belzberg A, Campbell JN (2010) Obturator nerve transfer as an option for femoral nerve repair: case report. Neurosurgery 66(6 Suppl Operative):375 discussion 375
Gutmann EYJ (1944) The re-innervation of muscle after various periods of atrophy. J Anat 78(1–2):15–43
Burnett MG, Zager EL (2004) Pathophysiology of peripheral nerve injury: a brief review. Neurosurg Focus 16(5):E1
Dumitru D (2000) Physiologic basis of potentials recorded in electromyography. Muscle Nerve 23(11):1667–1685
Dumitru D, King JC, Rogers WE, Stegeman DF (1999) Positive sharp wave and fibrillation potential modeling. Muscle Nerve 22(2):242–251
Dumitru D AA, Zwarts M (2001) Special Nerve Conduction Techniques. Elsevier.
Forman DS, Berenberg RA (1978) Regeneration of motor axons in the rat sciatic nerve studied by labeling with axonally transported radioactive proteins. Brain Res 156(2):213–225
Brown MC, Ironton R (1978) Sprouting and regression of neuromuscular synapses in partially denervated mammalian muscles. J Physiol 278:325–348
Fowler TJ, Danta G, Gilliatt RW (1972) Recovery of nerve conduction after a pneumatic tourniquet: observations on the hind-limb of the baboon. J Neurol Neurosurg Psychiatry 35(5):638–647
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study does not incorporate any sources of external funding or support.
Conflict of interest
Juan S. Uribe is a consultant for NuVasive, Inc. All other authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Ethical approval
This study is an institutional review board (IRB)-approved retrospective review of a prospectively collected database. The study protocol was approved by the IRB. All patient identifiable protected health information has been removed from the database used for the study.
Informed consent
Due to the retrospective nature for the study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Abel, N.A., Januszewski, J., Vivas, A.C. et al. Femoral nerve and lumbar plexus injury after minimally invasive lateral retroperitoneal transpsoas approach: electrodiagnostic prognostic indicators and a roadmap to recovery. Neurosurg Rev 41, 457–464 (2018). https://doi.org/10.1007/s10143-017-0863-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-017-0863-7