Abstract
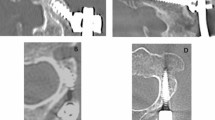
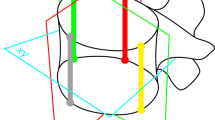
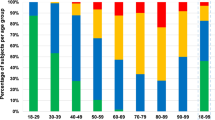
Pedicle screw fixation of the spine has become one of the most stable and versatile methods of spine fixation, and knowledge of pedicle morphology is crucial for the safe application of these systems. We undertook this study because only a few reports have investigated Eastern populations. Lumbar pedicle anatomy, i.e., pedicle width (PW) and pedicle height (PH), transverse and sagittal pedicle angles (TPA, SPA), and pedicle length (PL), were assessed in the following two groups: (1) computed tomography scans of 29 normal adults, and (2) 16 dried lumbar spines obtained from the Anatomy Department. Interpedicular distance was different in each group. PW ranged from 4 mm to 14 mm. In both groups, the narrowest PH was 8.2 mm, the widest 19.7 mm. TPA ranged from 6o to 19o and increased from L1 to L5. In the sagittal plane, the pedicles angled caudally at L5. PL was longest at L1 and shortest at L5. In conclusion, pedicle dimensions and angles may show individual and structural differences. Our data were not significantly different from previous reported data. A detailed knowledge of these relationships is important for any surgery involving screw purchase via a pedicle, to prevent screw cutout and failure of fixation or neurological injury. Selection of the proper diameter of screw is an important issue for safe placement. Knowledge of the pedicle axis length is essential in choosing screw lengths but should always be checked intraoperatively with fluoroscopic control during screw insertion.
Résumé
L'implantation de vis pédiculaires vertébrales est devenue une des méthodes de fixation de la colonne vertébrale les plus stables et polyvalentes. La connaissance de la morphologie pédiculaire est fondamentale pour une utilisation de ces implants en toute sécurité. Les populations orientales ont été peu étudiées, c'est pourquoi nous avons réalisé ce travail. L'anatomie du pédicule vertébral, c'est-à-dire la largeur pédiculaire (lP) et la hauteur pédiculaire (HP), l'inclinaison pédiculaire dans les plans transversal et sagittal (APT, APS), et la longueur pédiculaire (lP), a été évaluée dans les deux groupes suivants : (1) 29 examens tomodensitométriques d'adultes normaux et (2) 16 colonnes lombaires sèches appartenant à la collection du département d'anatomie. La distance interpédiculaire (DIP) était différente dans chaque groupe. La lP variait de 4 mm à 14 mm. Dans les deux groupes, la HP la plus étroite était de 8,2 mm, la plus large de 19,7 mm. L'APT variait de 6° à 19° et augmentait de L1 à L5. Dans le plan sagittal, les pédicules étaient inclinés caudalement au niveau de L5. Les LP étaient les plus élevées au niveau de L1 et les plus basses au niveau de L5. En conclusion, les dimensions et les inclinaisons pédiculaires avaient tendance à montrer des différences individuelles et structurales. Nos données ne sont pas significativement différentes des données rapportées par d'autres auteurs. Une connaissance détaillée de ces rapports est importante pour toute chirurgie proposant de choisir une vis par rapport à un pédicule, ceci dans le but de prévenir un trajet de vis extra-osseux et une défaillance de la fixation ou une lésion neurologique. La sélection du diamètre approprié de la vis est un point important pour un placement en toute sécurité. La connaissance de la longueur de l'axe pédiculaire est essentielle dans le choix des longueurs de vis, mais doit toujours être vérifié durant l'opération avec un contrôle radioscopique pendant l'insertion de la vis.


Similar content being viewed by others
References
Aebi M, Etter C, Kehl T, Thalgott J (1988) The internal skeletal fixation system: a new treatment of thoracolumbar fractures and other spinal disorders. Clin Orthop 227: 30–43
Berry JL, Moran JM, Berg WS, Steffee AD (1987) A morphometric study of human lumbar and selected thoracic vertebrae. Spine 12: 362–367
Blumenthal S, Gill K (1993) Complications of the Wiltse pedicle screw fixation system. Spine 18: 1867–1871
Chaynes P, Sol J-C, Vaysse P, Becue J, Lagarrigue J (2001) Vertebral pedicle anatomy in relation to pedicle screw fixation. Surg Radiol Anat 23: 85–90
Ciappetta P, Delfini R, Costanzo G (1996) Posterolateral decompression and stabilization of thoracolumbar injuries using Diapason instrumentation. Acta Neurochir (Wien) 138: 314–321
Denis F (1983) The three-column spine and its significance in the classification of acute thoracolumbar spinal injuries. Spine 8: 817–831
Gaines RW Jr (2000) The use of pedicle-screw internal fixation for the operative treatment of spinal disorders. J Bone Joint Surg Am 82: 1458–1476
Hou S, Hu R, Shi Y (1993) Pedicle morphology of the lower thoracic and lumbar spine in a Chinese population. Spine 18: 1850–1855
Kim NH, Lee HM, Chunk IH, Kim HJ, Kim SJ (1994) Morphometric study of the pedicles of thoracic and lumbar vertebrae in Koreans. Spine 19: 1390–1394
Krag MH, Beynon BD, Pope MH, Frymoyer JW, Haugh LD, Weaver DL (1986) An internal fixator for posterior application to short segments of the thoracic, lumbar or lumbosacral spine: design and testing. Clin Orthop 203: 75–98
Lee TC (1996) Transpedicular reduction and stabilization for postlaminectomy lumbar instability. Acta Neurochir (Wien) 138: 139–145
Loenstein JE, Denis F, Perra JH, Pinto MR, Smith MD, Winter RB (1999) Complications associated with pedicle screws. J Bone Joint Surg Am 81: 1519–1528
Luque ER (1986) Interpeduncular segmental fixation. Clin Orthop 203: 54–57
McCormack BM, Benzel EC, Adams MS, Baldwin NG, Rupp FW, Maher DJ (1995) Anatomy of the thoracic pedicle. Neurosurgery 37: 303–308
Nagel DA, Edwards WT, Schneider E (1991) Biomechanics of spinal fixation and fusion. Spine 16 (Suppl): S151–S154
Panjabi MM, Goel V, Oxland T, Takata K, Duranceau J, Krag M, Price M (1992) Human lumbar vertebrae. Quantitative three-dimensional anatomy. Spine 17: 299–306
Pihlajamäki H, Böstman O, Ruuskanen M, Myllynen P, Kinnunen J, Karaharju E (1996) Posterolateral lumbosacral fusion with transpedicular fixation. Acta Orthop Scand 67: 63–68
Robertson PA, Stewart NR (2000) The radiologic anatomy of the lumbar and lumbosacral pedicles. Spine 25: 709–715
Roy-Camille R, Saillant G, Mazel C (1986) Internal fixation of the lumbar spine with pedicle screw plating. Clin Orthop 203: 7-17
Scoles PV, Linton AE, Latimer B, Levy ME, Digiovanni BF (1988) Vertebral body and posterior element morphology: the normal spine in middle life. Spine 13: 1082–1086
Semaan I, Skalli W, Veron S, Templier A, Lassau J-P, Lavaste F (2001) Anatomie quantitative tridimensionnelle du rachis lombaire. Rev Chir Orthop 87: 340–353
Steffee AD, Biscup RS, Sitkowski DJ (1986) Segmental spine plates with pedicle screw fixation. A new internal fixation device for disorders of the lumbar and thoracolumbar spine. Clin Orthop 203: 45–53
Steinmann JC, Herkowitz HN, El-Kommos H, Wesolowski DP (1993) Spinal pedicle fixation. Confirmation of an image-based technique for screw placement. Spine 18: 1856–1861
Ullrich CG, Binet EF, Sanecki MG, Kieffer SA (1980) Quantitative assessment of the lumbar spinal canal by computed tomography. Radiology 134: 137–143
Whitecloud TS III, Butler JC, Cohen JL, Candelora PD (1989) Complications with the variable spinal plating system. Spine 14: 472–476
Yoganandan N, Larson SJ, Pintar F, Maiman DJ, Reinartz J, Sances A (1990) Biomechanics of lumbar pedicle screw/plate fixation in trauma. Neurosurgery 27: 873–881
Zindrick MR, Wiltse LL, Doornik A, Widell EH, Knight GW, Patwardan AG, Thomas JC, Rothman SL, Fields BT (1987) Analysis of the morphometric characteristics of the thoracic and lumbar pedicles. Spine 12: 160–166
Zindrick MR, Wiltse LL, Widell EH, Thomas JC, Holland WR, Field BT, Spencer CW (1986) A biomechanical study of intrapedicular screw fixation in the lumbosacral spine. Clin Orthop 203: 99–112
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kadioglu, H.H., Takci, E., Levent, A. et al. Measurements of the lumbar pedicles in the Eastern Anatolian population. Surg Radiol Anat 25, 120–126 (2003). https://doi.org/10.1007/s00276-003-0109-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-003-0109-y