Abstract
Purpose
Meta-analysis was conducted to estimate whether MiTLIF could reduce the complication rate while maintaining the similar clinical result to that of open procedures.
Methods
A search of the literature was conducted on pubmed or EMBASE. A database including patient clinical information was created. A systematic review of eligible studies with multivariate regression analysis was performed to quantitatively review the correlation of VAS improvement rate and the performance of MiTLIF.
Results
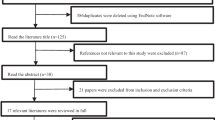
Fourteen articles with a minimum of 12-month follow-up met our inclusion criteria. The hypothesis of homogeneity could be accepted. The fixed-effects model was used to calculate the summary risk ratio (odds ratio). In the pooled analysis, the summary risk ratio (odds ratio) in patients with MiTLIF against those with open procedure for fusion rate, complication rate and revision/readmission rate was 0.99 (p = 0.36), 1.15 (p = 0.5) and 2.59 (p = 0.003), respectively, suggesting that MiTLIF was a risk factor for revision/readmission. Multivariate regression analysis showed that the percentage of male patients and the length of surgery exert a significant impact on VAS improvement rate. The selection of MiTLF was not significant.
Conclusion
Fusion rate and complication rate for both open and MiTLIF were similar. Moreover, the MiTLIF group tended to have a higher revision/readmission rate, which might be associated with the deep learning curve. Therefore, to achieve the level of surgical skill required of an MiTLIF surgeon, many years of training and experience are necessary. Otherwise, MiTLIF may yield unsatisfactory result upon patients.




Similar content being viewed by others
References
Kalanithi PS, Patil CG, Boakye M (2009) National complication rates and disposition after posterior lumbar fusion for acquired spondylolisthesis. Spine (Phila Pa 1976) 34(18):1963–1969
Tsutsumimoto T, Shimogata M, Ohta H, Misawa H (2009) Mini-open versus conventional open posterior lumbar interbody fusion for the treatment of lumbar degenerative spondylolisthesis: comparison of paraspinal muscle damage and slip reduction. Spine (Phila Pa 1976) 34(18):1923–1928
Rodriguez-Vela J, Lobo-Escolar A, Joven E, Munoz-Marin J, Herrera A, Velilla J (2013) Clinical outcomes of minimally invasive versus open approach for one-level transforaminal lumbar interbody fusion at the 3- to 4-year follow-up. Eur Spine J 22(12):2857–2863
Adogwa O, Parker SL, Bydon A, Cheng J, McGirt MJ (2011) Comparative effectiveness of minimally invasive versus open transforaminal lumbar interbody fusion: 2-year assessment of narcotic use, return to work, disability, and quality of life. J Spinal Disord Tech 24(8):479–484
Schizas C, Tzinieris N, Tsiridis E, Kosmopoulos V (2009) Minimally invasive versus open transforaminal lumbar interbody fusion: evaluating initial experience. Int Orthop 33(6):1683–1688
Peng CW, Yue WM, Poh SY, Yeo W, Tan SB (2009) Clinical and radiological outcomes of minimally invasive versus open transforaminal lumbar interbody fusion. Spine (Phila Pa 1976) 34(13):1385–1389
Wang J, Zhou Y, Zhang ZF, Li CQ, Zheng WJ, Liu J (2010) Comparison of one-level minimally invasive and open transforaminal lumbar interbody fusion in degenerative and isthmic spondylolisthesis grades 1 and 2. Eur Spine J 19(10):1780–1784
Shunwu F, Xing Z, Fengdong Z, Xiangqian F (2010) Minimally invasive transforaminal lumbar interbody fusion for the treatment of degenerative lumbar diseases. Spine (Phila Pa 1976) 35(17):1615–1620
Adogwa O, Parker SL, Bydon A, Cheng J, McGirt MJ (2011) Comparative effectiveness of minimally invasive versus open transforaminal lumbar interbody fusion: 2-year assessment of narcotic use, return to work, disability, and quality of life. J Spinal Disord Tech
Lau D, Lee JG, Han SJ, Lu DC, Chou D (2011) Complications and perioperative factors associated with learning the technique of minimally invasive transforaminal lumbar interbody fusion (TLIF). J Clin Neurosci 18(5):624–627
Park Y, Ha JW (2007) Comparison of one-level posterior lumbar interbody fusion performed with a minimally invasive approach or a traditional open approach. Spine (Phila Pa 1976) 32(5):537–543
Kotani Y, Abumi K, Ito M, Sudo H, Abe Y, Minami A (2011) Mid-term clinical results of minimally invasive decompression and posterolateral fusion with percutaneous pedicle screws versus conventional approach for degenerative spondylolisthesis with spinal stenosis. Eur Spine J
Kim DY, Lee SH, Chung SK, Lee HY (2005) Comparison of multifidus muscle atrophy and trunk extension muscle strength: percutaneous versus open pedicle screw fixation. Spine (Phila Pa 1976) 30(1):123–129
Zairi F, Arikat A, Allaoui M, Assaker R (2013) Transforaminal lumbar interbody fusion: comparison between open and mini-open approaches with two years follow-up. J Neurol Surg A Cent Eur Neurosurg 74(3):131–135
Harris EB, Sayadipour A, Massey P, Duplantier NL, Anderson DG (2011) Mini-open versus open decompression and fusion for lumbar degenerative spondylolisthesis with stenosis. Am J Orthop (Belle Mead NJ) 40(12):E257–E261
Lee KH, Yue WM, Yeo W, Soeharno H, Tan SB (2012) Clinical and radiological outcomes of open versus minimally invasive transforaminal lumbar interbody fusion. Eur Spine J 21(11):2265–2270
Villavicencio AT, Burneikiene S, Roeca CM, Nelson EL, Mason A (2010) Minimally invasive versus open transforaminal lumbar interbody fusion. Surg Neurol Int 1(12)
Stang A (2010) Critical evaluation of the Newcastle–Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605
Zdeblick TA (1998) Laparoscopic spinal fusion. Orthop Clin North Am 29(4):635–645
Sihvonen T, Herno A, Paljarvi L, Airaksinen O, Partanen J, Tapaninaho A (1993) Local denervation atrophy of paraspinal muscles in postoperative failed back syndrome. Spine (Phila Pa 1976) 18(5):575–581
McKinstry CS, Bell KE (1990) The failed back syndrome: the diagnostic contribution of computed tomography. Ulster Med J 59(2):122–130
Harrop JS, Youssef JA, Maltenfort M, Vorwald P et al (2008) Lumbar adjacent segment degeneration and disease after arthrodesis and total disc arthroplasty. Spine (Phila Pa 1976) 33(15):1701–1707
Goldstein CL, Macwan K, Sundararajan K, Rampersaud YR (2014) Comparative outcomes of minimally invasive surgery for posterior lumbar fusion: a systematic review. Clin Orthop Relat Res 472(6):1727–1737
Kim SS, Denis F, Lonstein JE, Winter RB (1990) Factors affecting fusion rate in adult spondylolisthesis. Spine (Phila Pa 1976) 15(9):979–984
Wu RH, Fraser JF, Hartl R (2010) Minimal access versus open transforaminal lumbar interbody fusion: meta-analysis of fusion rates. Spine (Phila Pa 1976) 35(26):2273–2281
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Q. Jin-tao and T. Yu contributed equally to this work.
Rights and permissions
About this article
Cite this article
Jin-tao, Q., Yu, T., Mei, W. et al. Comparison of MIS vs. open PLIF/TLIF with regard to clinical improvement, fusion rate, and incidence of major complication: a meta-analysis. Eur Spine J 24, 1058–1065 (2015). https://doi.org/10.1007/s00586-015-3890-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-3890-5