Abstract
Purpose
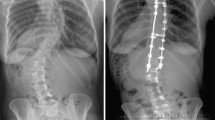
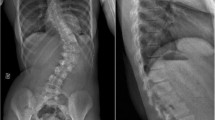
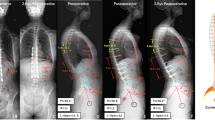
There are still no data proving whether restoring the ideal sagittal profile (according to Roussouly classification) in adult scoliosis (AS) patients leads to any additional benefit, especially regarding mechanical complications.
Methods
Retrospective analysis of operated AS patients recorded in a prospective multicenter database. Demographic and radiographic (preoperative and 6-week postoperative) data were analyzed. Patients with and without mechanical complications were compared looking especially at the surgical restoration of the ideal (based on Pelvic Incidence) sagittal profile. Univariate and multivariate analysis was performed to identify causes of mechanical complications at 2-year minimum follow-up.
Results
Ninty-six AS patients were analyzed. Thirty-nine patients suffered a mechanical complication (18 PJK, 11 pseudoarthrosis, 10 screw pull-out), and 57 patients had no mechanical complications. Postoperatively, 72% of patients not matching the ideal Roussouly-type suffered mechanical complications compared to 15% of matched patients (P < 0.001). Univariate analysis showed that older patients 64.9 ± 13 versus 40.7 ± 15.6 years (P < 0.001), higher postoperative Global Tilt (27° vs. 14.7°) and Pelvic Tilt (25° vs. 16°) (P < 0.001), upper instrumented vertebra at the thoracolumbar junction (62% vs. 21%) (P < 0.001), fixation to the Iliac (76% vs. 6%) (P < 0.001), and postoperative Roussouly-type mismatch (72% vs. 15%) (P < 0.001) significantly increased the rate of mechanical complications. Multivariate logistic regression analysis selected: postoperative Roussouly-type mismatch (OR = 41.9; 95%CI = 5.5–315.7; P < 0.001), iliac instrumentation (OR = 19.4; 95%CI = 2.6–142.5; P = 0.004), and age (OR = 1.1; 95%CI = 1.02–1.16; P = 0.004), as the most important variables.
Conclusions
Adult scoliosis surgery should restore the ideal Roussouly sagittal profile to decrease the rate of mechanical complications, especially in patients older than 65, instrumented to the pelvis.
Graphical Abstract
These slides can be retrieved under Electronic Supplementary Material.



Similar content being viewed by others
References
Aebi M (2005) The adult scoliosis. Eur Spine J 14:925–948. https://doi.org/10.1007/s00586-005-1053-9
Sebaaly A, Riouallon G, Obeid I et al (2018) Proximal junctional kyphosis in adult scoliosis: comparison of four radiological predictor models. Eur Spine J 27(3):613–621. https://doi.org/10.1007/s00586-017-5172-x
Scemama C, Laouissat F, Abelin-Genevois K, Roussouly P (2017) Surgical treatment of thoraco-lumbar kyphosis (TLK) associated with low pelvic incidence. Eur Spine J 26(8):2146–2152. https://doi.org/10.1007/s00586-017-4984-z
Barrey C, Darnis A (2015) Current strategies for the restoration of adequate lordosis during lumbar fusion. World J Orthop 6(1):117–126. https://doi.org/10.5312/wjo.v6.i1.117
Yilgor C, Sogunmez N, Boissière L et al (2017) Global alignment and proportion (GAP) score. J Bone Joint Surg Am 99(19):1661–1672. https://doi.org/10.2106/JBJS.16.01594
Barrey C, Jund J, Noseda O, Roussouly P (2007) Sagittal balance of the pelvis-spine complex and lumbar degenerative diseases. A comparative study about 85 cases. Eur Spine J 16:1459–1467. https://doi.org/10.1007/s00586-006-0294-6
Dubousset J (1994) Three-dimensional analysis of the scoliotic deformity. In: Weinstein SL (ed) The pediatric spine: principles and practice. Raven Press Ltd, New York, pp 479–496
Roussouly P, Gollogly S, Berthonnaud E, Dimnet J (2005) Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine 30:346–353
Laouissat F, Sebaaly A, Gehrchen M, Roussouly P (2018) Classification of normal sagittal spine alignment: refounding the Roussouly classification. Eur Spine J 27(8):2002–2011. https://doi.org/10.1007/s00586-017-5111-x
Sebaaly A, Grobost P, Mallam L, Roussouly P (2017) Description of the sagittal alignment of the degenerative human spine. Eur Spine J 27:489–496. https://doi.org/10.1007/s00586-017-5404-0
Pizones J, Martin MB, Perez-Grueso FJ et al (2019) Impact of adult scoliosis on Roussouly’s sagittal shape classification. Spine 44(4):270–279. https://doi.org/10.1097/BRS.0000000000002800
Takemoto M, Boissière L, Vital J-M et al (2017) Are sagittal spinopelvic radiographic parameters significantly associated with quality of life of adult spinal deformity patients? Multivariate linear regression analyses for pre-operative and short-term post-operative health-related quality of life. Eur Spine J 26(8):2176–2186. https://doi.org/10.1007/s00586-016-4872-y
Roussouly P, Pinheiro-Franco JL (2011) Biomechanical analysis of the spino-pelvic organization and adaptation in pathology. Eur Spine J 20(Suppl 5):609–618. https://doi.org/10.1007/s00586-011-1928-x
Sánchez-Mariscal F, Gomez-Rice A, Rodríguez-López T et al (2017) Preoperative and postoperative sagittal plane analysis in adult idiopathic scoliosis in patients older than 40 years of age. Spine J 17:56–61. https://doi.org/10.1016/j.spinee.2016.08.007
Yilgor C, Sogunmez N, Yavuz Y et al (2017) Relative lumbar lordosis and lordosis distribution index: individualized pelvic incidence–based proportional parameters that quantify lumbar lordosis more precisely than the concept of pelvic incidence minus lumbar lordosis. Neurosurg Focus 43:E5–E9. https://doi.org/10.3171/2017.8.FOCUS17498
Berthonnaud E, Dimnet J, Roussouly P, Labelle H (2005) Analysis of the sagittal balance of the spine and pelvis using shape and orientation parameters. J Spinal Disord Tech 18:40–47
Legaye J, Duval-Beaupère G, Hecquet J, Marty C (1998) Pelvic incidence: a fundamental pelvic parameter for three-dimensional regulation of spinal sagittal curves. Eur Spine J 7(2):99–103. https://doi.org/10.1007/s005860050038
Roussouly P, Pinheiro-Franco JL (2011) Sagittal parameters of the spine: biomechanical approach. Eur Spine J 20(Suppl 5):578–585. https://doi.org/10.1007/s00586-011-1924-1
Roussouly P, Nnadi C (2010) Sagittal plane deformity: an overview of interpretation and management. Eur Spine J 19:1824–1836. https://doi.org/10.1007/s00586-010-1476-9
Kim HJ, Bridwell KH, Lenke LG et al (2014) Patients with proximal junctional kyphosis requiring revision surgery have higher postoperative lumbar lordosis and larger sagittal balance corrections. Spine 39:E576–E580. https://doi.org/10.1097/BRS.0000000000000246
Sebaaly A, Sylvestre C, El Quehtani Y et al (2018) Incidence and risk factors for proximal junctional kyphosis: results of a multicentric study of adult scoliosis. Clin Spine Surg 31:E178–E183. https://doi.org/10.1097/BSD.0000000000000630
Charosky S, Guigui P, Blamoutier A et al (2012) Complications and risk factors of primary adult scoliosis surgery: a multicenter study of 306 patients. Spine 37:693–700. https://doi.org/10.1097/BRS.0b013e31822ff5c1
Lafage R, Schwab F, Challier V et al (2016) Defining spino-pelvic alignment thresholds: should operative goals in adult spinal deformity surgery account for age? Spine 41:62–68. https://doi.org/10.1097/BRS.0000000000001171
Liu F-Y, Wang T, Yang S-D et al (2016) Incidence and risk factors for proximal junctional kyphosis: a meta-analysis. Eur Spine J 25:2376–2383. https://doi.org/10.1007/s00586-016-4534-0
Clément J-L, Pelletier Y, Solla F, Rampal V (2018) Surgical increase in thoracic kyphosis increases unfused lumbar lordosis in selective fusion for thoracic adolescent idiopathic scoliosis. Eur Spine J 31:291–299. https://doi.org/10.1007/s00586-018-5740-8
Lonner BS, Parent S, Shah SA et al (2018) Reciprocal changes in sagittal alignment with operative treatment of adolescent Scheuermann kyphosis-prospective evaluation of 96 patients. Spine Deform 6:177–184. https://doi.org/10.1016/j.jspd.2017.07.001
Cecchinato R, Redaelli A, Martini C et al (2017) Long fusions to S1 with or without pelvic fixation can induce relevant acute variations in pelvic incidence: a retrospective cohort study of adult spine deformity surgery. Eur Spine J 26:436–441. https://doi.org/10.1007/s00586-017-5154-z
Kuklo TR, Bridwell KH, Lewis SJ et al (2001) Minimum 2-year analysis of sacropelvic fixation and L5-S1 fusion using S1 and iliac screws. Spine 26:1976–1983
Kim YJ, Bridwell KH, Lenke LG et al (2006) Pseudarthrosis in adult spinal deformity following multisegmental instrumentation and arthrodesis. J Bone Joint Surg Am 88:721–728. https://doi.org/10.2106/JBJS.E.00550
Acknowledgements
Johnson and Johnson DePuy-Synthes Spine and Medtronic research grant were received in partial support of this work.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study has institutional review board (IRB) approval/research ethics committee approval.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pizones, J., Moreno-Manzanaro, L., Sánchez Pérez-Grueso, F.J. et al. Restoring the ideal Roussouly sagittal profile in adult scoliosis surgery decreases the risk of mechanical complications. Eur Spine J 29, 54–62 (2020). https://doi.org/10.1007/s00586-019-06176-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-019-06176-x