Abstract
Summary: We report two cases of intraspinal extradural cysts communicating with an adjacent herniated disk that we term “disk cysts.” These cysts were well defined and homogeneous, and were present in the ventrolateral extradural space adjacent to a lumbar herniated disk. They had rim enhancement on contrast-enhanced MR images, and communication with a herniated disk was revealed by diskography.
Intraspinal extradural cystic lesions are uncommon. Intraspinal extradural cystic mass lesions include synovial cysts, ganglion cysts, Tarlov's perineural cysts, extradural arachnoid cysts, dermoid cysts, and neuromas with cystic changes. Among them, not one, to our knowledge, has been reported in association with herniated disks. We present two cases of intraspinal extradural cysts communicating with herniated disks.
Case Reports
Case 1
A 25-year-old woman had low back pain for 2 months, with progressive gait disturbance. A physical examination revealed decreased sensation in both lower extremities and motor weakness in the right lower extremity. MR imaging showed a small L3−L4 disk herniation (Fig 1A and B). An intraspinal cystic mass was depicted in the right lateral aspect of the ventral epidural space at the level of the L3−L4 disk down to the L4 vertebra, which displaced the dural sac dorsomedially. The mass was homogeneous and revealed intensities equivalent to those of CSF (Fig 1C and D). Contrast-enhanced MR images showed rim enhancement of the lesion (Fig 1E and F). Mild erosion of the posterior surface of the vertebral body adjacent to the cystic mass was noted. Some of the neurologic findings were not well explained by the extent of the herniated disk and the extradural cystic mass. Therefore, diskography and then CT diskography of the L3−L4 disk (Fig 1G and H) were performed and showed spilling of contrast material from the disk into the cystic mass.
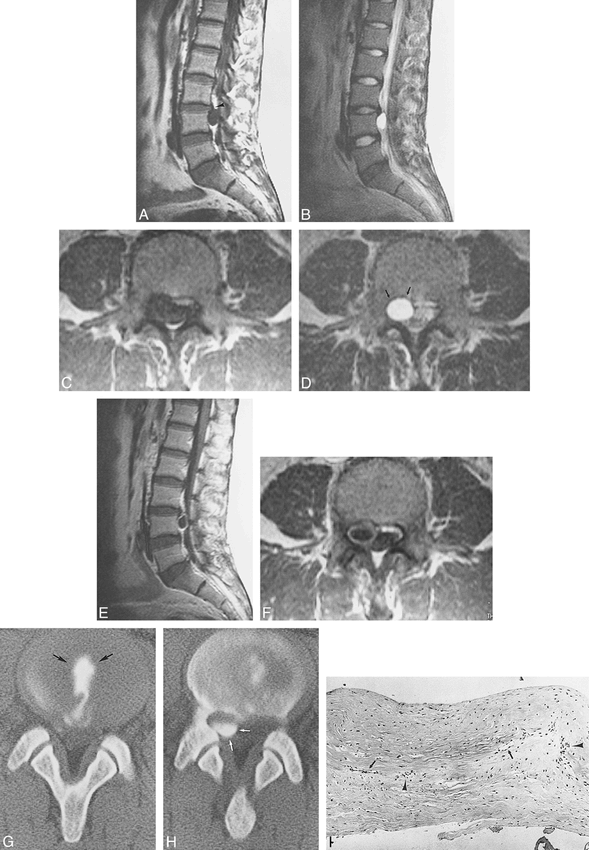
;t1Case 1: Disk cyst.
A, Sagittal T1-weighted image (right paramedian). A small L3−L4 herniated disk is seen (black arrowhead). Just below the herniated disk, a cystic mass is depicted with homogeneous low signal intensity.
B, Sagittal T2-weighted image (right paramedian). The cystic mass delineates homogeneous high intensity. The small L3−L4 herniated disk is just above the cyst.
C, Axial T1-weighted image at the cranial portion of the L4 level. Signal intensity of the cystic mass is equal to that of CSF.
D, Axial T2-weighted image at the cranial portion of the L4 level (same level as that shown in C). The cystic lesion displaces the dural sac dorsomedially. Erosion of the posterior margin of the L4 vertebral body (small arrows) is seen.
E, Enhanced sagittal T1-weighted image. The cyst shows rim enhancement.
F, Enhanced axial T1-weighted image (same level as that shown in C) shows rim enhancement of the cyst.
G, CT scan at L3−L4 after diskography. The contrast material is present in the L3−L4 disk (arrows).
H, CT scan at L4 after diskography. The contrast material spills out of the disk space and accumulates at the right dorsal aspect of the upper L4 body level (white arrows), corresponding to the cyst seen on the MR image.
I, Histologic section of the cyst wall (hematoxylin and eosin; original magnification, × 25). The cyst wall is composed of fibrous connective tissue without synovial cells or hemosiderin. Vascular proliferation (arrows) and a few lymphocytes (black arrowheads) are seen.
At surgery, a cyst that compressed the right L4 nerve root was found in the right ventral extradural space. The cyst contained clear fluid and communicated with the herniated disk at L3−L4 through a small hole. The cyst and herniated disk were removed. The posterior longitudinal ligament appeared normal, and the lateral membrane, which runs continuously from the posterior longitudinal ligament, was not recognized. A histologic examination of the cyst wall revealed fibrous connective tissue without synovial cells or hemosiderin (Fig 1I). Vascular proliferation and a few lymphocytes were seen in the fibrous connective tissue. After surgery, low back pain and the right leg motor weakness disappeared. Abnormal sensation remained on the lateral aspect of the right lower extremity.
Case 2
A 29-year-old man complained of low back pain for 3 months and experienced decreased sensation in both lower extremities without motor weakness. MR imaging depicted a small L4−L5 disk herniation (Fig 2A) and a cystic mass in the right lateral aspect of the ventral extradural space from the level of the herniated disk down to the L5 vertebra. The dural sac was displaced dorsally. The mass was homogeneous and isointense compared with CSF (Fig 2B). Contrast-enhanced MR imaging showed rim enhancement of the lesion (Fig 2C). Myelography and CT myelography failed to show a communication between the CSF space and the cystic lesion. Diskography and then CT diskography of the L4−L5 disc were performed. Diskography and CT diskography (Fig 2D and E) showed that contrast material flowed from the involved disk into the cystic mass.
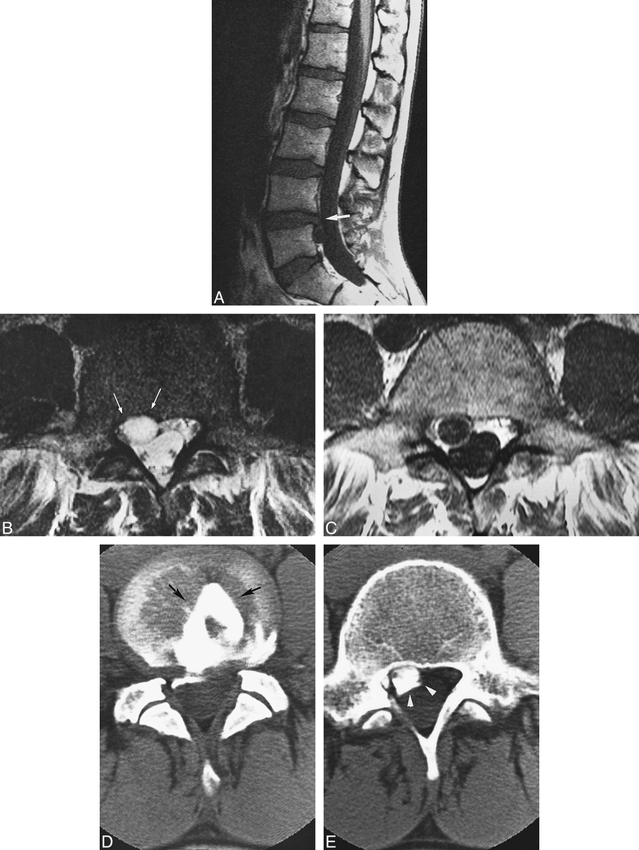
;t1Case 2: Disk cyst.
A, Sagittal T1-weighted image (right paramedian). A small herniated L4−L5 disk is seen (large white arrow). Just below the herniated disk, a cystic mass is visible.
B, Axial T2-weighted image just below the L4−L5 level. A cystic mass is present in the right anterior extradural space. The dural sac is slightly deformed by this mass. Mild erosion of the right posterior bony wall of L4 is seen (white arrows). The lesion is nearly isointense with CSF.
C, Enhanced axial T1-weighted image (same level as that shown in fig 2B). The mass exhibits rim enhancement.
D, CT diskography at the L4−L5 level depicts water-soluble iodine contrast material in the L4−L5 disk (arrows).
E, CT diskography at the L5 level. Contrast material spills over and accumulates in the right anterior epidural space (white arrowheads).
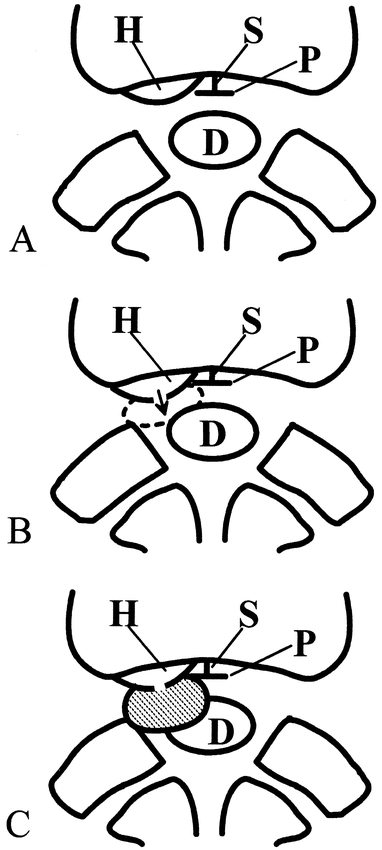
Illustration of proposed mechanism of disk cyst formation.
A, Herniated disk (H) develops.
B, Fluid is generated by the herniated disk material (arrow). The dotted line indicates a pseudomembrane.
C, Relation of the herniated disk and a disk cyst. The hatched area indicates a disk cyst. The interruption of the disk cyst wall indicates the communication between the cyst and herniated disk.
(S, midline septum; D, dural sac; P, posterior longitudinal ligament.)
A right laminotomy was performed at L4−L5. A cyst was seen adjacent to the right posterior surface of the L5 vertebra, compressing the right L5 nerve root dorsally. The cyst communicated with the involved disk through a small hole and contained faintly brown fluid. The cyst and the small extruded L4−L5 herniated disk were resected. A microscopic examination of the cyst wall showed fibrous connective tissue without synovial cells. After surgery, the patient's low back pain and right leg sensory deficit disappeared; however, abnormal sensation remained on the lateral aspect of the left lower extremity.
Discussion
In 1997, a report was published in the Japanese language literature that corresponded to the type of cases discussed herein (1). Because these cysts communicate with herniated disks, we designate them “disk cysts.” In our search, we found no English-language reports concerning such cysts. A disk cyst is a well-defined homogeneous cyst, present in the ventrolateral extradural space adjacent to a lumbar herniated disk, which displaces the dural sac dorsomedially. It may erode an adjacent vertebral body. On MR images, the cystic mass was homogeneous and isointense compared with CSF. Contrast-enhanced MR imaging delineated rim enhancement of the lesion. Diskography and CT diskography of the involved disk revealed that the cyst filled with contrast material through the herniated disk.
Although the mechanism of disk cyst formation is unknown, two hypotheses have been suggested. One theory implicates epidural hematoma because the cyst content was hemorrhagic fluid in four of the seven cases reported by Toyama et al (1). This theory suggests that an epidural hematoma is produced by rupture of the epidural vein by mechanical irritation from a herniated disk. According to Toyama et al, the hematoma eventually becomes a disk cyst. Intraspinal epidural hematomas have been reported (2), and their imaging findings are similar to the findings in our cases regarding their location and their well-defined cystic nature. According to this report, it seems that no contrast-enhanced MR imaging or diskography was performed and that communication between the cyst and the disk was not documented. Cyst content was serous in one of our cases and faintly brown in the other, and the microscopic findings of the cyst walls showed no hemosiderin, which does not support the epidural hematoma theory.
We prefer another hypothesis, in which a disk cyst results from focal degeneration and cystic softening of collagenous connective tissue of the disk with fluid production, similar to the mechanism of meniscal cyst formation occasionally observed in patients with meniscal degeneration in the knee (3). An intervertebral disk degenerates, a herniated disk develops, and there is spilling of fluid from the herniated disk material in selected cases. We assume that reactive pseudomembrane formation subsequently develops and that the fluid is encapsulated, thus causing a meniscal cyst eventually to form. The histologic findings of the cyst wall, including fibrous structure without synovial lining cells, in our cases, are compatible with pseudomembrane. Cystic fluid may be serous or may contain protein to some degree because the fluid is assumed to come from degenerative disk material.
The clinical and radiologic differential diagnosis of intraspinal extradural cystic mass lesions includes synovial cyst, ganglion cyst, Tarlov's perineural cyst (4), extradural arachnoid cyst (5), dermoid cyst, and neuroma with cystic changes. A synovial cyst develops from a facet joint, is usually on the posterolateral aspect of the dural sac, contains mucinous fluid, and has synovial lining cells in its wall. An intraspinal synovial cyst can be differentiated from a disk cyst by location (6). Intraspinal ganglion cysts, the origin of which is disputed, are usually referred to as cysts arising from the facet joints of the lumbar spine and are found in the dorsolateral epidural space. Histologically, the wall of a ganglion cyst is made up of connective tissue without synovial lining cells. Although its histologic findings are identical to those of a disk cyst, a ganglion cyst usually is differentiated from a disk cyst by location. Some ganglion cysts, however, have been reported to be in the ventrolateral extradural space. A case of an intraspinal ganglion cyst has been reported with CT myelographic findings similar to those of our cases, which included bony erosion of the posterolateral aspect of a vertebral body and dorsomedial displacement of the dural sac (7). The cyst wall in that case was composed of loose stroma with stellate cells without epithelial lining. MR findings for a ganglion cyst in another report documented a smooth oval-shaped mass, and the cyst wall was enhanced on T1-weighted contrast-enhanced images (8). These two cases seem difficult to differentiate from disk cysts; however, it may be that they were disk cysts. If diskography had been performed in these latter two cases, communication between the cyst and an involved disk might have been revealed.
Tarlov's perineural cysts are extradural meningeal cysts, which are often multiple and may occur along the dorsal nerve roots at any level. The nerve fibers lie within the cyst wall or lie within the cyst itself. These cysts do not usually enhance on contrast-enhanced MR images (9). These extradural meningeal cysts probably communicate with the subarachnoid space at some point during their development, and communication can be seen with CT myelography (10). Bone erosion has been reported in the posterior vertebral bodies in the sacrum. We probably can exclude these extradural meningeal cysts, because they do not have peripheral rim enhancement on contrast-enhanced CT scans or MR images unless they are complicated by inflammation.
The microscopic findings for extradural arachnoid cysts can be practically identical with those for disk cysts. Arachnoid cysts, however, occur predominantly in younger persons and are located primarily in the thoracic spine and usually in the dorsal aspect of the dural sac (5). Rim enhancement of arachnoid cysts is not expected on contrast-enhanced MR images.
Neuromas with cystic changes may have findings similar to those of disk cysts on MR images, but practically, the overwhelming majority of neuromas with cystic change reveal areas of nodular or thicker enhancement that are different from what is seen in our two cases.
Our two disk cysts and the seven reported in the Japanese literature were not located in the midline but instead in the ventrolateral extradural space. Because the lateral membrane was not recognized during surgery in our cases, it is not clear whether the disk cyst was present ventral to the lateral membrane (ventral epidural space). The ventral epidural space is a space between the lateral membrane and the periosteum and normally contains a venous network embedded in the areolar tissue (11). There is a septum in the ventral midepidural space, which connects ventrally with thickened periosteum and dorsally with the posterior longitudinal ligament (11). Therefore, we think that disk cysts do not develop in the midline, as in cases of sequestered herniated disks, because the posterior longitudinal ligament prevents the cyst from developing dorsally to it.
Because we encountered two patients with disk cysts in a short period, we assume that disk cysts are not rare and may have been treated previously, or reported as epidural hematomas or ganglion cysts. When an intraspinal cyst is observed in the ventrolateral extradural space on MR images or CT myelographic scans, the possibility of a disk cyst should be considered. Diskography is thus useful in obtaining a correct preoperative diagnosis of disk cyst.
Footnotes
1 Address reprint requests to Kinuko Kono, MD, Department of Radiology, Osaka City University Medical School, 1–5–7 Asahimachi, Abeno, Osaka 545–8585 Japan.
- Received October 6, 1998.
- Accepted after revision February 17, 1999.
- Copyright © American Society of Neuroradiology